Painful sex is more common in women. The cause may be physical or psychological, and is often a combination of the two. A painful experience of sex may lead to anxiety the next time, poor relaxation and lubrication, and so sex is painful again, and so on. If anxiety is great, the vaginal muscles may go into spasm, blocking penile entry completely. This is called vaginismus, and is fully discussed below.
Painful sex in men usually has a physical cause – commonly a skin infection of some sort on the skin of the penis. Other rarer causes are discussed below.
PAINFUL SEX IN WOMEN
The medical term ‘dyspareunia’ describes the condition when intercourse is painful, but possible. It is very common, and most women will have had at least some experience of it during their sexual lives. It is one of the most common complaints women make when they consult a gynaecologist, or a doctor in a sexual health clinic.
Occasionally a woman may be too shy to mention it and hope the doctor brings it up (which they may or may not do), or complain instead about another symptom, such as heavy periods. This is unfortunate, as the symptom of painful sex, if it occurs, can be helpful to doctors trying to reach a diagnosis.
CAUSES OF DYSPAREUNIA
Doctors divide dyspareunia into two categories: superficial or deep.
If the pain occurs when the penis enters the vagina, and is concentrated around the entrance to the vagina, it is called superficial dyspareunia.
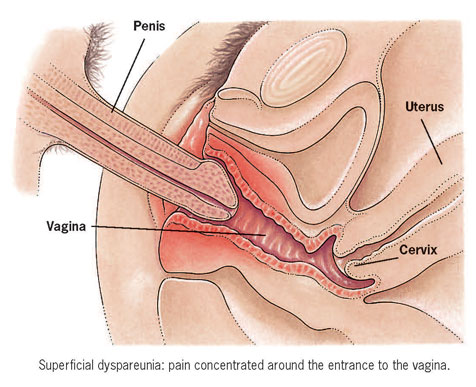
If the penis can be inserted comfortably but the pain occurs ‘deep’ in the lower abdomen, when the penis is fully inserted, it is called deep dyspareunia.

Both may occur together. If penile entry is impossible because the vaginal muscles go into a painful spasm, it is called vaginismus.
Infections (superficial or deep):
Thrush (candida), trichomoniasis, genital herpes and low-grade bacterial infections are common causes of painful sex. Symptoms can include:
• A change in the colour, smell and amount of vaginal discharge
• Itching or pain
• The appearance of blisters or pimples, which may burst and discharge clear fluid, blood or pus.
Other infections, such as infection caused by chlamydia and gonorrhoea, are less common, but can lead to inflammation of the cervix and the pelvic organs, causing deep dyspareunia.
If an infection is suspected, a full check-up at a sexual health clinic (sexually transmitted infection/STI or special clinic) will be necessary. The appropriate treatment can then be prescribed.
As a general rule it is best to avoid washing the genital area with anything other than water because soaps, shower gels, bubble baths and disinfectants strip the vagina of healthy bacteria and allow other forms of infection to take hold.
Sex may be painful for a while even after the infection has cleared, because of remaining inflammation and reduced lubrication.
Postnatal or postsurgical problems (superficial or deep):
The shape of the vagina may be altered after giving birth, particularly if the vagina was torn or cut, and then stitched. The scar that forms may not stretch as much as the rest of the vagina, making sex painful.
Women can resume intercourse after birth as soon as they wish, and as soon as tears or episiotomies have healed. Some women resume as early as two weeks after delivery, although others prefer to wait till their first postnatal check. Women may find their libido changed (either increased or decreased) and that sex feels quite different compared to before they were pregnant, because of the stretching of the vaginal muscles.
The vaginal area may also be affected by operations for incontinence or vaginal prolapse. In some cases it may be possible for the surgeon to refashion scarred areas to allow for easier intercourse.
Problems with the cervix, uterus, tubes or ovaries (deep):
The following common gynaecological conditions can all cause deep pain on intercourse:
• Pelvic inflammatory disease (an inflammation of the uterus and tubes caused by infection)
• Fibroids: these are fibrous growths in the uterus. They may be single or multiple and cause pain as they increase in size
• Endometriosis (the growth of uterine tissue outside the uterus, which also bleeds during periods)
• Ovarian cysts: these may grow progressively larger, and pressure during intercourse leads to pain
Associated problems may include heavy, painful or irregular periods. If symptoms also include bleeding between periods or after intercourse, or lower abdominal pain and weight loss, tumours of the cervix or pelvic organs need to be ruled out.
Women should always be up to date with their cervical smears, and go to their GP for examination and investigation. A referral for an ultrasound scan and a gynaecological opinion may be necessary.
Insufficient lubrication (superficial):
Women who have prolonged or vigorous intercourse or frequent intercourse (several times daily) may suffer pain during sex simply as a result of friction. Lubrication with a water-based lubricant (e.g. KY Jelly) can help ease this problem, but it may be an idea to cut down on sex till it feels more comfortable. Remember also that oil-based lubricants (such as massage oils, Vaseline, cooking oil, etc.) can damage rubber and lead to condom accidents.
Women also vary greatly in the amount of lubrication they produce, even when sexually excited, and again the use of additional lubrication can make sex more comfortable.
Vaginal dryness and thinning of vaginal tissue is one effect of the menopause. Menopausal women should therefore use additional lubrication or consider hormone replacement therapy either locally to the vagina or for the whole body.

Having sex for the first time (superficial and/or deep):
Women having sex for the first time can find the experience painful, especially if the hymen has not been previously broken by tampons or other instruments. This is compounded by anxiety, lack of experience (of both partners), lack of arousal and therefore lubrication, and clumsiness or forcefulness by the male partner.
Anxiety can be dealt with by the following:
• Having sufficient information about the sexual act
• Being prepared beforehand for the prevention of pregnancy and sexually transmitted infections (with a condom and the oral contraceptive pill for instance)
• Being relaxed with one’s surroundings and one’s partner
• Making sure there is plenty of lubrication before penile entry is attempted.
Lubricants (e.g. KY Jelly, from the pharmacist) can be used safely with condoms. Most oils (cooking oil, massage oil, Vaseline) break condoms.
It may help if penetration is attempted slowly, in stages, with the introduction of one finger, and then two, beforehand. It may take several episodes of intercourse for the woman to relax fully and become used to the sensation of having her vagina stretched by the penis.
Problems with the structure of the vagina or hymen (superficial):
Some women have a particularly small vaginal opening, which becomes painful when stretched. In other women the hymen, which is normally torn during first intercourse, is stiff, and does not tear completely, giving rise to pain. Or it may split on two sides, leaving a hard band in the middle, which again makes sex uncomfortable. A few women have a ‘septate vagina’, in which their vagina is divided lengthways with a partition of tissue – this can of course lead to painful intercourse.
A physical examination by a doctor will rule out these unusual shapes, and in most cases simple surgery will rectify the problem.
Psychological causes:
As sex for women involves penetration, it is often important that it takes place in an atmosphere of relaxation and trust. Any anxiety (about their own sexuality, pregnancy, the relationship, etc.) can lead to tensing of the vaginal muscles and painful intercourse.
The woman may also become tense in response to a physical cause of pain, or a remembered trauma, e.g. childbirth or rape. Severe anxiety can lead to vaginismus which is discussed below. If a psychological cause is suspected, relationship or psychosexual counselling may be useful.
Vaginismus
Vaginismus is defined as uncontrollable tightening of the lower vaginal muscles, so that attempted penile entry is painful and impossible. In some cases the thigh muscles clench as well, so that the partner is unable to get near the vagina.

Vaginismus can range from the ability to use tampons and tolerate a vaginal examination but not to have sex, to the inability to touch or insert anything into the vagina without provoking the reaction.
Vaginismus is the most common cause of non-consummation of marriage and is thought to occur in about five of every thousand women, and makes up between 5 and 42 per cent of the sex therapist’s workload.
Vaginismus may be caused by any of the reasons for painful sex listed above, if pain and anxiety are severe enough. It may occur after a traumatic experience of sex, such as rape or sexual abuse.
In cases where there are no obvious precipitants, and the woman has not experienced intercourse, vaginismus is usually the result of uncertainty and misinformation about the sexual act and about female genitalia. There may also be deeply held religious beliefs or the guilty view that sex and nakedness are ‘dirty’.
Vaginismus is best treated with the help of an understanding GP or a sex therapist.
A gentle examination is required to rule out physical problems. Once this has been done, the woman is encouraged to express her fears or fantasies about her body, proceeding to an exploration of her own genitalia. Her partner may be present if she so wishes.
Once she is aware of which muscles tense and how to relax them, the therapist will demonstrate that gentle insertion of a finger is possible. The woman is then encouraged to explore her vagina with her own fingers, or with ‘vaginal trainers’ of different sizes. The couple may then proceed to exercises in which the woman controls penile penetration, before full intercourse.
The outlook is extremely good, and sex therapists find this a rewarding condition to treat. In mild cases, only a few visits may be necessary, but in severe cases more sessions may be needed.
PAINFUL SEX IN MEN
Painful sex in men is almost always related to a physical cause – psychological problems lead instead to difficulties with erection. Common causes include the following.
Trauma
Vigorous or prolonged intercourse can cause small tears in the foreskin and head of the penis (glans). Infection will make these more inflamed and painful.
Tight foreskin
Some men have difficulty retracting their foreskins, and erection may lead to tightness and discomfort. It may also be difficult to clean the area behind the foreskin, and any resulting infection will add to the problem. Circumcision should be considered if problems are frequent.
An occasional complication of a tight foreskin is called paraphimosis – in which the man is unable to bring the foreskin down again after erection. The foreskin forms a tight band around the penis, which swells and becomes painful. It is important to go to an accident and emergency department immediately in these cases, because permanent damage can result if the condition is left unseen to.

Infections and skin reactions
Herpes infection causes painful, itchy blisters on the penis, which burst after a few days and scab over. Warts look like tiny cauliflowers on the skin.
Men can also get thrush, most commonly if their partners have it, and this causes irritation with redness and occasionally swelling at the head of the penis. A thick white discharge may collect underneath the foreskin.
Gonorrhoea and non-specific urethritis can cause both a burning sensation in the urethra with discharge, and pain on urination and ejaculation. If any of these infections are suspected, a full check-up at a sexual health clinic is necessary.
Some men are allergic to the rubber or lubricant used in ordinary condoms. Hypoallergenic condoms are now available from leading brands. It is also possible to react to massage oils, washing powders, shower gels or soaps.
Less common causes
Congenital deformities that cause bending of the penis with erection can cause pain. In a condition known as Peyronie’s disease, a lump of fibrous tissue develops along the shaft of the penis, and causes a painful asymmetrical erection. The condition may resolve by itself over months or years, but help should be sought if intercourse is impossible. Surgery is the answer for some men. In both cases the opinion of a urologist may be helpful.
Some men develop great sensitivity in the glans of the penis after ejaculating, which can be so severe that the man fears to do it. Young men also sometimes have an over-active cremaster muscle (the muscle that causes the scrotum to contract) and this can produce spasmodic pain during sex. A long period of arousal without ejaculation can also produce an aching sensation in the groin.
Priapism is a condition in which the erection fails to subside and lasts for hours, becoming painful. Urgent treatment at an accident and emergency department should be sought, because permanent damage can result.
KEY POINTS
-
If sex is painful, mention it to the doctor
-
For women, painful sex may be superficial, deep or both
-
Causes of painful sex in women are physical or psychological
-
Vaginismus (preventing penile entry) can be overcome with the help of a sex therapist
-
In men, painful sex is usually caused by a skin problem
