Types of stroke
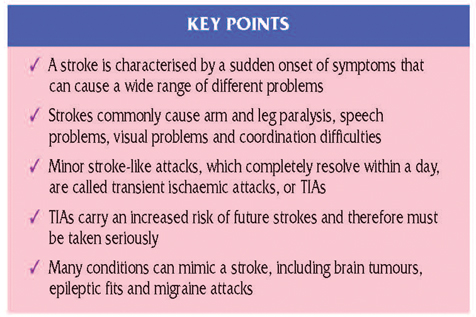
The symptoms of a stroke depend on which part of the brain has been damaged. Any part of the blood vessel system can become blocked so there are infinite varieties of stroke. The blood supply to the brain also varies a surprising amount from person to person. Some people can block three of their four main arteries and not have a stroke. Others may have a devastating stroke with a blockage of just one of the four arteries. This has led to great difficulty in classifying strokes and there are many different classifications in use around the world.
A STROKE ON THE LEFT SIDE OF THE BRAIN
A stroke affecting the right side of the body is usually the result of problems in the left side of the brain (and vice versa). For more details on the functions of the left and right side of the brain, see ‘What is a stroke?’.
The most familiar type of stroke is when someone suddenly develops a weakness of the right side of their face, arm and leg. This problem is easy to spot, and the medical term is a ‘hemiparesis’ or a ‘hemiplegia’ (commonly shortened to ‘hemi’). The weakness can vary from very mild to complete paralysis. It most often affects the face, arm and leg together, but some small strokes just affect the face alone or just the arm or the leg. Less commonly, strokes can cause just a loss of feeling (or sensation) in the face, arm or leg, or a mixture of a loss of feeling and weakness.

Although weakness is the obvious initial symptom of a stroke, the increased stiffness that develops later can cause many other problems. This stiffness is called spasticity and occurs in muscles that have lost their nerve supply and are not used regularly. If people do not get good rehabilitation after their stroke, the spasticity can lead to painful spasms and abnormal posture. Physiotherapy aims to restore normal movements and the early sessions often concentrate on reducing any spasticity of the affected arm and leg.
If your only problem after a stroke is a weakness down one side of your body, this suggests that the stroke has been slight and only damaged a small area of ‘wiring’ deep in your brain. If, however, the stroke has damaged a much larger area of your brain, other things are affected too.
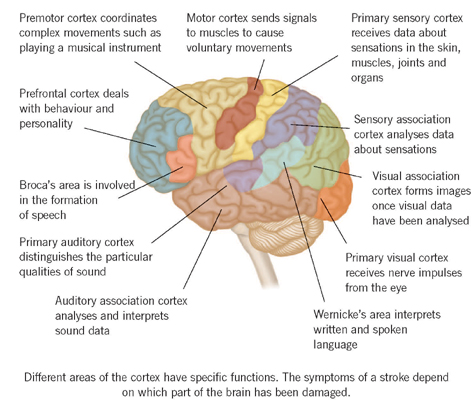
In right-handed people, the left side of the brain also controls language, an ability to see the world on the right, and an ability to recognise and coordinate things on the right. Therefore, larger strokes affecting the left side of the brain can cause a more severe combination of right-sided weakness, an inability to speak and an inability to see objects to the right. In left-handed people, these functions are usually controlled by the right side of the brain, although this is not an absolute rule.
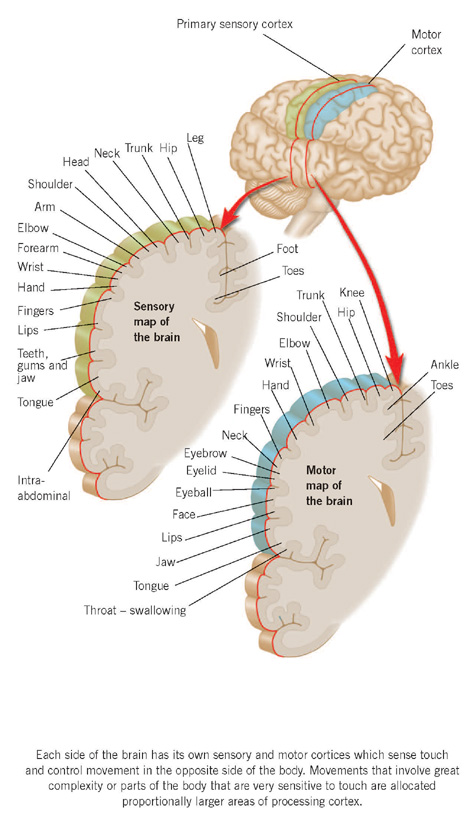
Case history
A retired managing director suddenly collapsed while standing in the kitchen. He fell onto the tiled floor and bruised himself badly.
He didn’t lose consciousness and managed to shout for help. When seen at the stroke unit, his mouth had drooped down on the right and he couldn’t move his right arm or leg at all. His speech was normal and he could feel normal sensations down the right side of his body. A brain scan using a technique called computed tomography (CT) showed a small area of damage deep in the left side of his brain, consistent with a blockage affecting a small blood vessel. His weakness rapidly improved and, after four weeks of rehabilitation at the stroke unit, he went home almost independent and able to climb stairs.
PROBLEMS AFFECTING SPEECH
Speech problems that occur with a stroke commonly involve a difficulty in mentally formulating and understanding the right words to use. People who recover from the language problem tell of the frustration it causes. Patients say that they knew that people were talking to them, but they couldn’t understand a word that was said. Similarly, they knew what to say but were unable to get the words out in the right order. This can be very mild, such as an inability to recall the name of a common object such as a watch, or more severe and mean a complete loss of all speech. Sometimes, a different type of speech problem occurs as a result of weakness of the muscles involved in moving the mouth and tongue when articulating words – this is known as dysarthria.

Case history
A retired teacher aged 70 was talking to her daughter on the telephone. Her daughter reported that her mother’s speech suddenly changed to ‘gibberish’ yet her mother was unaware of the problem. Mrs Smith had just had a stroke affecting the part of the brain that controls the production of speech. This symptom is called dysphasia.
A STROKE ON THE RIGHT SIDE OF THE BRAIN
The left side of the body is controlled by the right side of the brain and in right-handed people this is normally the non-dominant side. The problems are very similar to the ‘right-sided’ problems described above, but language problems are much less common.
One common problem seen in people with larger strokes affecting the left side of the body is that they often appear very disabled and it is difficult to see why at first. This problem is the result of a failure of the brain to recognise that the left arm and leg actually belong to that person. The part of the brain that tells you that you have a left arm and leg is so damaged that your brain assumes that you don’t have a left-hand side. When this is really severe, people can even ignore food on the left side of their plate, and ‘lose’ their left arm and leg.
Another pattern recognised in people with a left-sided weakness is abnormal speech, when the speech becomes rather monotonous or flat. The sing-song nature of speech that makes conversation more interesting and animated seems to be controlled by the right (or non-dominant) side of the brain.
Left-handedness
If you are naturally left-handed, the dominant side of your brain could be on the right or the left. Left-handed people may have a slightly different combination of stroke symptoms to those described above.
PROBLEMS AFFECTING VISION
The most common problem affecting eyesight is an inability to see the world on the right (or the left) as a result of problems in the brain on the left (or the right). This is because vision from the left field (side) of both eyes is controlled by the right side of the brain and vice versa. This loss of a visual field is often mistaken for blindness in an eye, but in fact it involves a loss of vision in one field of both eyes. This type of visual field loss is called a hemianopia. However, most strokes do not damage the eye, but affect the processing of information from the eye. Double vision can also be caused by a stroke if the balance and coordination centre of the brain is affected, although many other non-stroke conditions can also cause double vision.
PROBLEMS AFFECTING BALANCE
The base of the brain has a complicated set of ‘wiring’ and control mechanisms to stop you falling over. Strokes affecting this area of the brain can cause sudden unsteadiness, and many patients say the problem is just like being drunk.
TRANSIENT ISCHAEMIC ATTACKS
Some stroke symptoms disappear very quickly and within minutes (or hours) you are back to normal. If the stroke symptoms last less than 24 hours, doctors call the attack a transient ischaemic attack (TIA), a sort of mini-stroke. If the symptoms last more than 24 hours, the name ‘stroke’ is preferred. A TIA may be caused by a small blood clot that quickly breaks up, or a temporarily reduced blood flow in the brain (for example, as a result of an abnormal heart rhythm, low blood pressure or spasm of narrowed blood vessels).
A special form of a TIA affects the vision in one eye. This is called amaurosis fugax, or transient monocular blindness. A typical attack is when the vision in one eye disappears as if a black shutter was coming up or down. The attacks are sometimes described as a sudden misting of vision. You can test whether the problem is in both eyes or just the one eye by covering each eye in turn.
If your loss of vision is affecting just one eye and your vision recovers in seconds or minutes, this is usually the result of circulation problems affecting the blood supply to your eye (which is shared by your brain). The blood clot usually comes from a particular source, such as damage or disease affecting the heart or the carotid arteries (the blood vessels supplying blood to the head). These sorts of attacks can also be a warning of a future stroke, because the next time the blood clot may go to the brain, and not the eye.
A TIA is not a trivial attack and is a warning that there may be problems with the circulation. People who have had a TIA have a greater than normal risk of another attack which may be more serious, for example, a disabling stroke. It is therefore important that any stroke-like attack should be assessed by your doctor, who may be able to suggest ways of preventing more serious attacks in the near future.
Case history
A 65-year-old woman was smoking a cigarette when she suddenly dropped it. When she tried to pick it up, she found that her right hand was weak and she couldn’t grip her fingers tight enough. When she tried to get up out of the chair, she noticed that her right leg wasn’t moving. She waited five minutes and tried again, and managed to get to the telephone and call her son. When the son arrived 30 minutes later, she had regained full power in her hand and leg and felt back to normal. She had experienced a TIA, which can be an early warning of a more serious stroke yet to come.
CONDITIONS THAT MIMIC A STROKE
Many conditions can mimic a stroke, including the following.
Brain tumours
The main characteristic of a stroke is that the symptoms come on very quickly. A brain tumour can cause exactly the same problems as a stroke, but the symptoms tend to start gradually and get worse over days and weeks. Stroke-like symptoms that get worse need urgent medical attention from your doctor.
Migraine
Migraine is a very common condition, and some people experience a variety of symptoms with their attacks, with flashing lights, holes in their vision and even occasional arm or leg weakness. This can sometimes be difficult to treat and control, and some migraine attacks can be mistaken for a stroke. To complicate matters further, on rare occasions a migraine attack can lead to a stroke. An expert medical opinion may help in this situation.
Pins and needles
The sensation of pins and needles is a very common symptom and is only rarely caused by a stroke. More commonly, these symptoms are the result of a trapped nerve and have nothing to do with a stroke.
Eye symptoms
Symptoms such as a temporary loss of vision, blurred vision or double vision could result from a stroke, but are also signs of other serious problems affecting the eye. These symptoms should be assessed urgently by your family doctor. ‘Floaters’, small moving shapes that sometimes move across your vision, are not the result of a stroke and are usually normal.
Fits (or seizures)
These can occasionally mimic a stroke. Major fits often start with a collapse, and the person is unresponsive. The person’s arms and legs jerk in a rhythmical manner for a few minutes, followed by a quieter recovery period. The fit may cause incontinence of urine or faeces, and sometimes people find that they have bitten their tongue. Some people have a weakness just like a stroke immediately after a fit and, if the doctor wasn’t aware of the full attack, they may mistakenly diagnose a stroke. A witness can be very important to tell the two events apart, especially if a typical epileptic fit is seen.

