The uterus: structure, function and common problems
What is the uterus?
The uterus, referred to since Biblical times as the ‘womb’, is a very remarkable organ, capable of expanding to contain a full-grown baby and of shedding its lining up to 500 times during your life at the time of your monthly period.
The resultant stresses and strains on its supporting structures during pregnancies and the repeated shedding and re-growth of its lining may lead to problems such as prolapse or heavy menstrual bleeding. This chapter describes what the normal uterus and its related structures look like and how they work, and summarises what may go wrong.
When you’re not pregnant, your uterus is approximately pear-sized. It has a thick muscular wall and a central cavity with a lining that is richly supplied with blood vessels. This lining is known as the endometrium and it provides nourishment for the embryo during the very early days of life. Otherwise, the lining of the uterus is shed each month, resulting in a flow of blood lasting for several days. This is known as the menstrual flow, menstruation or the monthly period.
The location of the uterus within the pelvis
The uterus sits centrally in the pelvis supported by strong fibrous structures called ligaments
The uterine muscle wall expands greatly during pregnancy and strong contractions of this muscle wall during childbirth give rise to the pains of labour. You experience similar contractions on a much smaller scale during menstruation, and this is the cause of the period pain (dysmenorrhoea) which troubles so many women.
The cervix
The cervix (or neck of the uterus) is the link between the uterus and the vagina (or birth canal) and is found at the top of the vagina. It is a firm, smooth, rounded structure with a central opening which:
- dilates (opens up) during labour
- allows menstrual blood to flow through it during your periods
- allows sperm to travel through it into your uterus during sexual intercourse.
When a doctor needs to look at your cervix, this can easily be done by inserting an instrument called a speculum into your vagina, and most women are used to having this done when their doctor performs routine smear tests.
The fallopian tubes and ovaries
The ovaries are situated on either side of the pelvis and are white, slightly knobbly and grape-sized. They are extremely important because they are the source of eggs and also of the hormones, oestrogen and progesterone (see below), which control the menstrual cycle.
Each month an egg is released from one of the two ovaries in turn by a process called ovulation. This occurs at around day 14 of the menstrual cycle. The egg then enters the adjoining fallopian tube, one of two long, delicate structures attached to the uterus. This is where the egg may meet up with sperm if you have had sexual intercourse, so beginning a pregnancy.
A woman is born with a full supply of immature eggs and, from puberty onwards, these eggs gradually mature so that one is released each month until the egg supply finally runs out at the time of the menopause (see below).
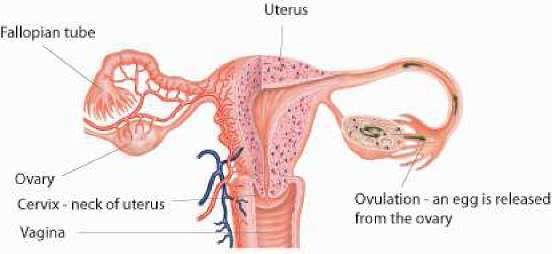
The female reproductive system
The ovaries which contain eggs are situated at either side of the uterus and are connected to it by the fallopian tubes. They produce oestrogen and prgesterone, hormones that control the menstrual cycle.
Supporting structures
The uterus and cervix sit centrally in the pelvis, at the top of the vagina, supported by strong fibrous structures called ligaments. These ligaments are attached in turn to the bones of the pelvis. They are sufficiently elastic to allow them to stretch considerably during pregnancy and then return to their former size afterwards.
In some women, particularly those who are past the menopause and those who have had children, this elasticity is reduced and the ligaments are weakened, leading to prolapse, or descent, of the uterus and cervix. This causes discomfort, a dragging sensation and an awareness of a swelling or bulge at the vaginal opening.
In front of the vagina and close to the cervix is the bladder, which stores then gets rid of urine through a short narrow passageway called the urethra. Behind the vagina is the rectum (back passage) where the bowel expels faeces. These organs are supported by ligaments and muscles that stretch during pregnancy and childbirth.
The pelvic floor
The ligaments and muscles that support the uterus, bladder and rectum, together with the walls of the vagina, are referred to as the ‘pelvic floor’. When you’re pregnant, you’re taught how to exercise the muscles of your pelvic floor and improve their strength once you’ve had your baby. Women who have a pelvic operation will need to do the exercises too as they help to prevent any weakness developing and so keep the bowels and bladder working properly.
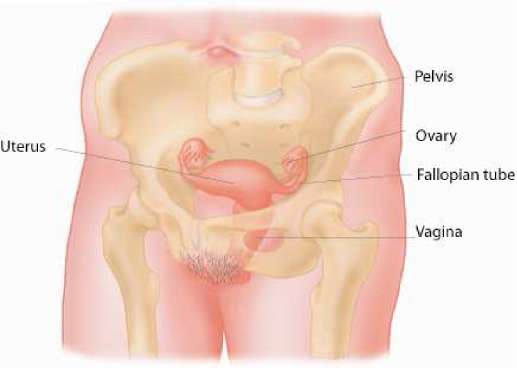
Inside the female pelvis
The female reproductive organs lie in the pelvis. At the lower end of the uterus the cervix leads into the vagina. At the top end two opening lead into the fallopian tubes, which lead to the ovaries.

The menstrual cycle
For around 40 years (on average, between the ages of 12 and 52), you experience monthly menstrual bleeding from the uterine lining, except for those times when you may be pregnant or breast-feeding.
The average length of the menstrual cycle is 28 days but it is quite normal for it to vary between 24 and 35 days and occasionally longer. Most women find that the bleeding is accompanied or preceded by crampy pain (dysmenorrhoea or period pain), caused by uterine contractions. It may also be preceded by mood changes, bloating and breast tenderness, now referred to as the premenstrual syndrome (PMS) and formerly called premenstrual tension (PMT).
These symptoms are caused by the hormones produced in the ovaries, which act mainly on the uterus but also have effects elsewhere in the body. Different societies vary in their views about menstruation and, within all societies, individual women have vastly different experiences of their monthly periods. However, most look on menstruation as an unwelcome, albeit necessary, process.
Female hormones
Oestrogen is the main female hormone produced by the ovaries and is responsible for the thickening of the uterine lining during the menstrual cycle. It also affects the vagina, breasts, bones and other tissues (for example, walls of blood vessels).
Progesterone, the other female hormone, is produced only after the egg is released at ovulation and acts on the lining of the uterus, thickening it in preparation for a possible pregnancy. If you don’t conceive that month, your hormone levels fall and your period starts.
The production of hormones and release of eggs from the ovaries are controlled by a small gland in the brain, called the pituitary gland, which regulates the length of the menstrual cycle.

The menopause
The menopause is the last menstrual period experienced by a woman. It occurs, at an average age of 52 in most Western countries. It happens when the supply of eggs in the ovaries eventually runs out.
It may be sudden or gradual; some women experience increasing irregularity of their periods for months or even years in the lead-up to the menopause (a time of transition known as the “perimenopause”).
As your supply of eggs declines, your hormone levels start to fall and this is what may cause the symptoms of hot flushes, night sweats, vaginal dryness and mood fluctuations that trouble many women. For most women, these symptoms are transient but a few find that they are a serious problem for quite a long time.
If this happens to you, your doctor may suggest treating the symptoms with hormone replacement therapy (HRT). Having your your ovaries surgically removed at the time of hysterectomy is likely to aggravate these problems and this issue is discussed later in the book.
Common disorders of the uterus and menstrual cycle
Given the total number of menstrual cycles experienced by most women, it is not surprising that menstrual problems occur frequently. These comprise painful periods, heavy periods, irregular bleeding and the premenstrual syndrome (PMS). Fibroids and endometriosis are common gynaecological disorders which may cause menstrual problems.
Bleeding problems are particularly common in the lead-up to the menopause (see below). Excessive bleeding is not only inconvenient, uncomfortable and embarrassing, it may also lead to anaemia (shortage of iron caused by blood loss).
Even after the menopause, the problems are not all over because this is the time when many women experience problems with prolapse of the uterus or vaginal walls. In particular, older women are more at risk of development of cancer of the uterine lining, cervix or ovaries, although fortunately these conditions are not common.
Information about the disorders which may affect the uterus and menstrual cycle is outlined below, and you will find more details on several of them in later chapters.
Heavy menstrual bleeding
Most women who seek medical help because of heavy periods have no serious cause for the bleeding and the problem is put down to a disorder of the shedding and re-growth of the uterine lining – so-called dysfunctional uterine bleeding.
Menstruation is a very complex process and one that is not yet fully understood. It is likely that repeated menstrual cycles lead to disorders in this process because periods tend to get heavier and less regular as women get older.
In some cases, the problem is related to changes in the levels of hormones produced by the ovaries in the lead-up to the menopause. Another factor may be that some women become very intolerant of their periods once they have completed their families and are less prepared to put up with the monthly discomfort and inconvenience.
Investigations described in the next chapter may identify a cause for the bleeding. In the absence of an obvious cause, decisions about treatment must depend largely on the severity of the symptoms, the impact they are having on the lifestyle and commitments of the individual woman, and whether heavy bleeding has led to anaemia (a low blood count which must be treated with iron tablets).
You should always be offered medical treatment in the first instance (see page xx). One of the most effective treatments is the Intrauterine System or IUS (see page xx). This may be available at your GP’ surgery, a family planning clinic or the hospital outpatient clinic.
Endometrial ablation is a minor surgical procedure which is done under local or general anaesthetic in the hospital outpatient clinic or day surgery unit (see page xx).
If these measures fail, removal of the uterus, hysterectomy, albeit rather drastic, will guarantee permanent relief but, as major surgery is involved, the risks as well as the benefits must always be fully considered (see page xx).
Bleeding in between periods
Some women experience unexpected bleeding which occurs in between their normal menstrual periods. If this is heavy, prolonged or persistent it must be reported to a doctor as it may require urgent investigation. It is also important to report any bleeeding which occurs during or immediately after sexual intercourse (post coital bleeding). This may be caused by an infection or abnormality of the cervix.
The most serious cause is cervical cancer athough this is unlikely if you have always had regular smears. Minor bleeding or spotting in between periods is unlikely to have a serious cause. Some women have slight bleeding in the middle of their cycle or in the lead up to each period. If this bleeding is light and regular it is most likely to be due to hormone changes but if in doubt always consult your doctor. Irregular bleeding or spotting may be a side effect of some hormonal treatments such as contraceptives or hormone replacement therapy.
This is known as “break through bleeding. Usually women are warned to expect this in the first few months of any treatment but if bleeding is heavy or fails to settle a pelvic examination and possibly other investigations, described in the next chapter, will be required.
Persistent bleeding in between periods may be caused by hormonal changes or by a polyp (fleshy swelling) or fibroid (see below) attached to the uterine lining. These abnormalities can be detected by ultrasound or hysteroscopy (page xx) and can usually be removed by minor surgery.
Abnormal bleeding and the menopause
It is very common for women to experience changes in their menstrual cycles in the lead up to the menopause (see page xx) and this can cause worry and confusion, particularly if you don’t know whether or when to expect another period.
Many women consult their doctors because of bleeding problems related to the perimenopause (transition time over the menopause) and if these are due to hormonal fluctuations they are usually easy to treat. However diseases of the uterus, including cancer, are also more common as women get older and your GP may arrange referral to a hospital clinic for further investigation.
Any bleeding which occurs 12 months or more after your last menstrual period must be reported to a doctor without delay as it may be a sign of cancer. Fortunately over 80% of women who experience bleeding after the menopause do not have cancer. Common causes of bleeding after the menopause include late periods, polyps, thinning of the vaginal wall leading to inflammation (atrophic vaginitis) and bleeding related to HRT.
Uterine fibroids
One of the most common causes of heavy bleeding is enlargement and distortion of the uterus by rounded outgrowths of the muscle wall called fibroids. These are benign (non-cancerous) tumours and vary in size, number and position.
If they are very large they may cause pressure on the bowel or bladder; if small they may not cause any symptoms. They can be detected by abdominal or pelvic examination and confirmed by an ultrasound scan. Heavy periods caused by fibroids may be treated medically (see page xx), but this is less successful if the fibroids are numerous or large because medical treatments will not permanently shrink the fibroids. Similarly, use of an IUS or endometrial ablation may not be possible or is less likely to succeed if there are large fibroids.
A newer, non-surgical alternative is uterine artery embolisation (see page xx). Fibroids can be removed individually without removing the whole uterus (myomectomy – see page xx) if you want to have children in future.
Fibroids will shrink naturally after the menopause but if this is some years away and you are troubled by symptoms such as heavy bleeding or pelvic pressure, hysterectomy will give you the best guarantee of a cure.
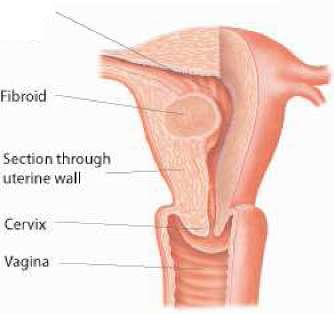
Uterine fibroids
Fibroids can grow in the wall of the uterus and they are one of the most frequent causes of heavy bleeding
Menstrual pain
Menstrual pain is caused by a combination of contractions of the muscle of the uterine wall and spasm of the blood vessels supplying the uterine lining. Most women experience pain with their periods but the degree of pain is extremely variable for reasons which are not well understood.
In most cases period pain (known as dysmenorrhoea) responds to simple medical treatments, such as pain-killers or the oral contraceptive pill. Severe pain associated with menstruation, which is not relieved by standard medical treatments, may be caused by endometriosis (see below and page xx). Another condition, more common in older women who have had children, is ‘pelvic congestion syndrome’ in which periods are both painful and heavy with a build-up of pain, including backache and painful intercourse, in the lead-up to the period.
Similar symptoms are caused by adenomyosis (see page xx) a condition related to endoemtriosis. Hormonal therapies including the ‘pill’ can be successful by blocking ovulation and the hormone changes that follow.
Hormones can also be used to stop the menstrual cycle altogether. Hysterectomy is a possible option in severe cases. Some women with pelvic pain have underlying problems such as stress or depression which may be aggravating the menstrual problem.
It is important to appreciate that if pelvic pain is not related to the menstrual cycle and is not relieved by hormones, it is not likely to improve after a hysterectomy.
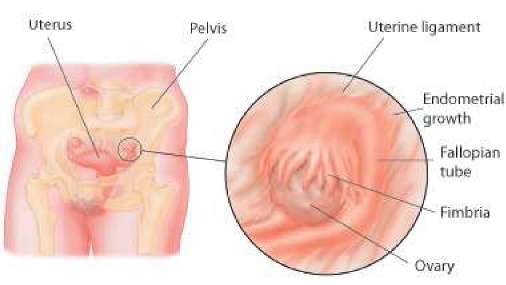
Endometriosis
Endometriosis arises because some women shed a little of the lining of their womb through their fallopian tubes into the pelvis during menstruation. This is more likely to occur in women who have heavy and painful periods. Small patches of uterine lining tissue (endometrium) may grow on the ligaments behind the uterus, on the walls of the pelvis or on the ovaries.
These patches then respond to the hormone changes of the menstrual cycle, giving rise to additional pain before or during menstruation. This may also cause deep discomfort or pain during intercourse and interfere with fertility.
Endometriosis may be detected during a pelvic examination or by a scan but usually a laparoscopy is needed to make a definite diagnosis (see page xx). The symptoms of endometriosis are usually treated successfully with medical treatment (see page xx) or sometimes with minor “keyhole” surgery (page xx) but in the longer term the condition may recur and removal of the ovaries and uterus is a possible long-term solution.
In cases of severe endometriosis, the patches of endometriosis may cause adhesions (scar tissue) in the pelvis, causing the uterus and ovaries to stick to each other and to nearby organs , such as the bowel and bladder. This can make any form of surgery potentially difficult and the endometriosis may be difficult to remove completely.
Severe endometriosis may be a cause of infertility and this may make the decision to have a hysterectomy difficult for those women who are hoping to have one or more children in the future. In this situation, it is particularly important that all alternative options are fully considered.
Endometriosis
Fragments of the endometrium (lining of the womb) sometimes travel from the uterus into the pelvic cavity via the fallopian tubes. They then may implant on parts of the pelvic organs causing the structures to stick together.
Adenomyosis
This condition causes heavy and painful periods as a result of the presence of uterine lining tissue in the uterine muscle wall, causing the uterus to be tender and bulky. In contrast to endometriosis, which is more common in women who have not had children, adenomyosis usually occurs in women who have had several pregnancies.
It may develop as a complication of endometrial ablation. It can be treated medically but hysterectomy may be recommended if medical treatments are not successful. The diagnosis of adenomyosis is difficult to make on the basis of standard investigations because it is not always visible on ultrasound scanning, and cannot be detected by hysteroscopy or endometrial biopsy. Most cases are confirmed only after a hysterectomy has been performed and the uterus examined by a pathologist.
Uterine prolapse
A uterine prolapse is the descent of the uterus and cervix so that they no longer sit up at the top of the vagina, but can be felt lower down, sometimes as far down as the vaginal opening.
Prolapse of the uterus is caused by weakness of its supporting structures, usually as a consequence of child-bearing. You are most likely to develop it after rather than before the menopause and it is usually accompanied by prolapse of the vaginal walls.
When it happens, you experience a dragging sensation and you and/or your doctor may feel a smooth swelling at the vaginal opening. Some women tolerate a prolapse for many years and come to no harm, but it can be a considerable nuisance and restrict your activities unnecessarily. If it is very large, the skin over the prolapse may become irritated by contact with underclothing, leading to discharge and even bleeding.
Minor degrees of prolapse may not require an operation or may be treated by a pelvic floor repair which leaves the uterus intact. However, removal of the uterus through the vagina (vaginal hysterectomy) together with repair of the pelvic floor is usually recommended if the prolapse is large.
When a woman develops a prolapse before she has had all the children she would like, she will usually be advised to delay having surgical treatment until her family is complete. A ring pessary can be fitted as a temporary measure to support the pelvic floor. Ring pessaries are also suitable for the treatment of women who are not well enough to undergo an operation or for those keen to avoid surgery.
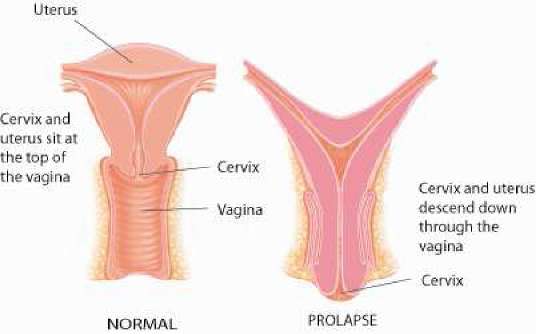
Uterine prolapse
In uterine prolapse the uterus is displaced and moves down into the vagina. This normally occurs when the ligaments in the pelvis become weakened, usually as a result of childbirth or after the menopause.
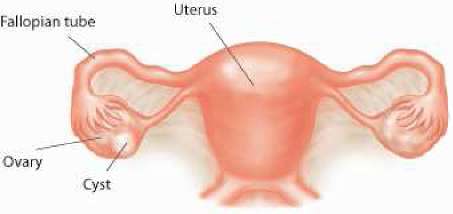
Ovarian cysts and tumours
An ovarian cyst is a collection of fluid within the ovary. Small cysts, measuring between 3 and 5 cm, commonly develop as a complication of the menstrual cycle and normally do not require any treatment because they go away on their own.
Larger cysts can be drained or removed without removing the ovary. If the ultrasound scan shows that the cyst is made up of solid areas as well as fluid, or if there is a solid swelling on the overy (an ovarian tumour), it may be necessary to remove the whole ovary.
If the cyst is very large or if there is doubt about its nature, the gynaecologist may recommend removal of the uterus and the other ovary, provided that you do not wish to have any more children. This is especially likely if there is concern that the cyst may be malignant (cancerous). Although most ovarian cysts are benign, there is a greater risk of cancerous changes if it is very large.
Scans and blood tests are helpful in predicting whether an ovarian cyst is malignant. There is also a small risk that a similar cyst may develop at a later stage in the other ovary. More information is given about the treatment of ovarian cancer in a later chapter.
Ovarian cysts
An ovarian cyst is a sac full of fluid that grows on or near an ovary. Surgical removal may be necessary if it is very large or if there is concern that it may be malignant.
Premenstrual syndrome
Most women are aware of changes in mood along with their menstrual cycle. There are also physical changes such as bloating and breast tenderness which commonly occur in the lead up to a period. These are put down to the normal hormone changes of the menstrual cycle but in some women the mood and physical changes are more severe; known as premenstrual syndrome or PMS.
The cause of PMS is not known as women who suffer from this do not have abnormal levels of hormones. Women with other menstrual problems such as heavy or painful periods often find that their PMS improves with treatments such as hormones, the IUS or endometrial ablation but these are unlikely to help if PMS is the only or main problem.
Stress is thought to aggravate symptoms of PMS and some women respond to non medical approaches. Treatment with drugs which alter the level of the chemical serotonin in the brain can also be helpful in severe cases. These drugs are known as SSRIs and are used for the treatment of depression. Examples are fluoxetine (Prozac) and paroxetine (Seroxat). They can be taken cyclically rather than continuously to reduce mood swings of PMS.
Some women with very severe PMS benefit from removal of their ovaries, but this is a very drastic measure and does not guarantee a cure.
Long-term treatment with hormone replacement therapy (HRT) is essential for women who lose their ovaries at a young age. Some women with PMS are unusually sensitive to the effects of hormones and have difficulty with HRT (for more on medical treatments, see page xx).
KEY POINTS
- The menstrual cycle is controlled by the hormones oestrogen and progesterone, produced by the ovaries
- A woman sheds her uterine lining each month during menstruation – up to 500 times in her lifetime
- Common problems include heavy bleeding, menstrual pain, mood swings (PMS), fibroids, endometriosis and prolapse of the uterus
- Bleeding disorders are especially common near the menopause because of changes in hormone production by the ovaries