Treating infertility
Many infertility problems don’t require assisted conception techniques, such as in vitro fertilisation (IVF), but can be treated with simpler methods. The treatments you will be offered will depend on the cause of your infertility. If you are not ovulating properly, you may be offered either medication to correct the cause or fertility drugs to stimulate the ovaries.
If you have blocked or damaged fallopian tubes, you may need surgery, either as an open operation or, increasingly, by laparoscopy (‘keyhole’ surgery). Disorders of sperm function respond poorly to drug treatment. Instead, you may be offered sperm donation or assisted conception (for more details, see later sections). Drug treatment for endometriosis does not improve fertility.
OVULATION INDUCTION
If you are not ovulating or do so irregularly, your chances of conceiving are obviously diminished. There are several causes of ovulation failure, and most cause either a complete absence of menstrual periods (amenorrhoea) or infrequent periods (oligomenorrhoea). Provided you have not gone through an early menopause, the available treatments are generally very effective.
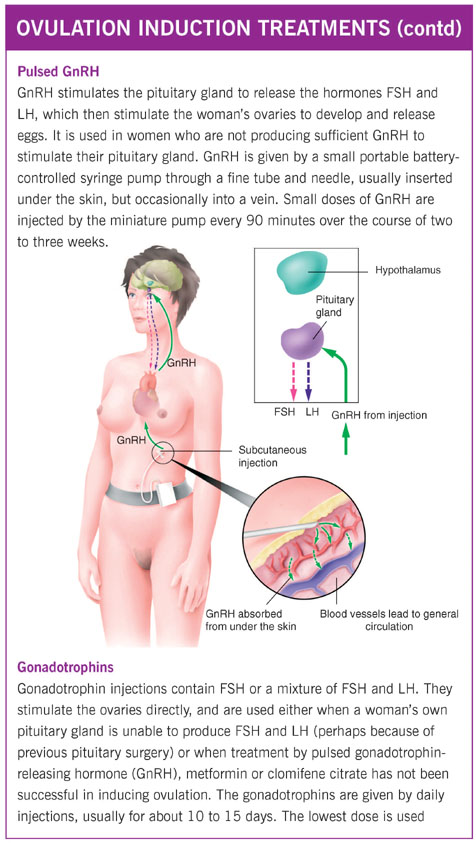
Some conditions that may require more complex medical treatment or, occasionally, even surgical treatment include: hypopituitarism (underactivity of the pituitary gland, which leads to less follicle-stimulating hormone (FSH) and luteinising hormone (LH) being produced); hypogonadotrophic hypogonadism (poor ovarian activity caused by inadequate stimulation of the pituitary gland); hyperprolactinaemia (excessive prolactin hormone production by a small benign (non-cancerous) tumour of the pituitary gland) and polycystic ovary syndrome (where the hormone signals to the ovaries are unbalanced, leading to development of multiple immature egg sacs).
If your periods have stopped because of excessive or sudden weight loss, you may respond to dietary measures alone, but most other causes of ovulation failure are likely to require specific hormone treatments. The methods used to induce ovulation include metformin, clomifene citrate, bromocriptine and cabergoline, pulsed GnRH, gonadotrophin therapy and ovarian diathermy.
Women with ovulation failure caused by a premature menopause will not respond to ovulation induction treatments. However, their problem can be bypassed by using donated eggs for IVF. For more details of these treatments, see ‘Assisted conception’.
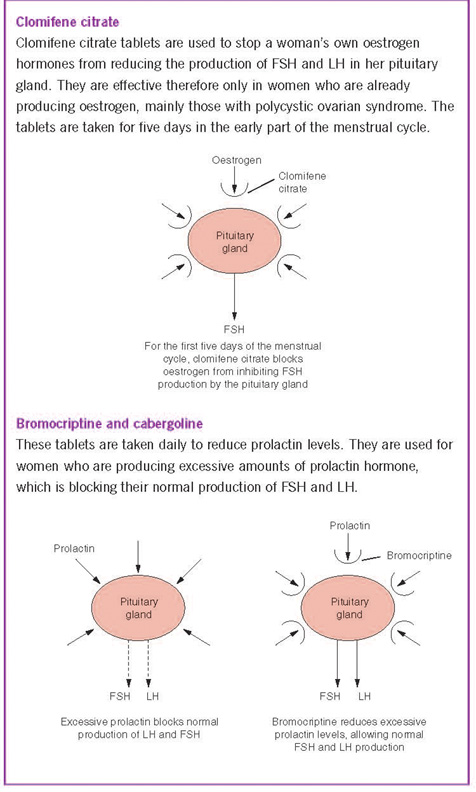


Using metformin for polycystic ovary syndrome
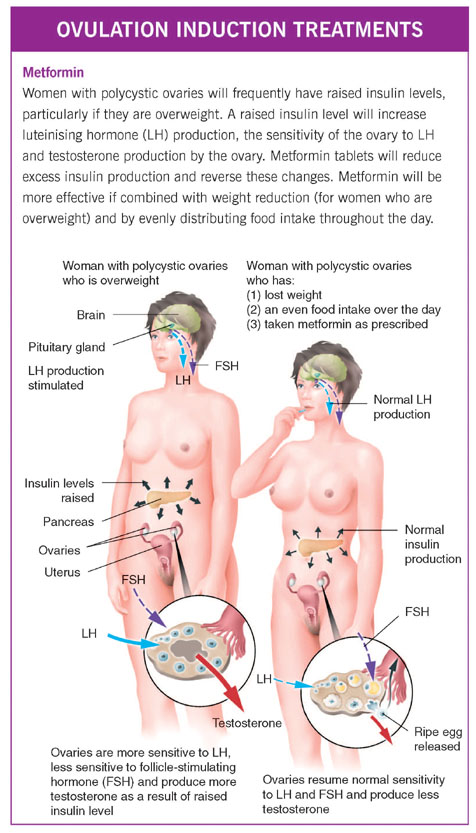
Metformin is a drug that has previously been used extensively in the treatment of type 2 diabetes, that is, the form that does not require treatment with insulin. Metformin is not a hormone itself, but is now increasingly used in the management of polycystic ovary syndrome (PCOS). It is of particular benefit if the woman’s weight is excessive. It reduces the excess amount of insulin in the circulation and acts in several ways, including an improvement in how efficiently cells throughout the body can use glucose to produce the energy that they need. Extensive research in women with PCOS has shown that metformin is effective in correcting the hormone imbalance that they have, which can otherwise stop ovulation or interfere with egg quality. By reducing excessive insulin levels, metformin will also reduce the increased levels of luteinising hormone (LH) and testosterone which are present in the circulation of women with PCOS.
Metformin treatment is believed to improve the coordination of events at the time an egg is released, which improves egg quality and probably increases the length of time during which it can be fertilised. Metformin has also been shown to increase blood flow to the lining of the uterus in women with polycystic ovaries, which may improve the chance of an embryo implanting normally.
Metformin is likely to be more effective if combined with other simple measures of reducing any excess insulin production. These include weight reduction for women who are overweight, regular exercise and evenly distributing food intake throughout the day, but in particular avoiding a large meal at the end of the day, which can otherwise cause a prolonged rise in insulin levels.
Within six months of starting metformin treatment, women whose cycles are absent or infrequent have been found to get a return to normal regular cycles in more than 90 per cent of cases, and more than 20 per cent of these women have been reported to conceive. Metformin is an important new addition to the management of infertility associated with PCOS. It is often used in combination with clomifene citrate.
The risk of ovarian cancer
There are concerns about whether the use of clomifene or gonadotrophins may lead to increased risks of ovarian cancer later in life. These risks are difficult to quantify, partly because women with ovulation failure may have a slightly increased risk of ovarian cancer anyway, but also because a pregnancy from any successful treatment greatly reduces the risk of ovarian cancer.
The evidence available at present does not suggest that these treatments increase the risk of ovarian cancer when used appropriately.
TUBAL SURGERY
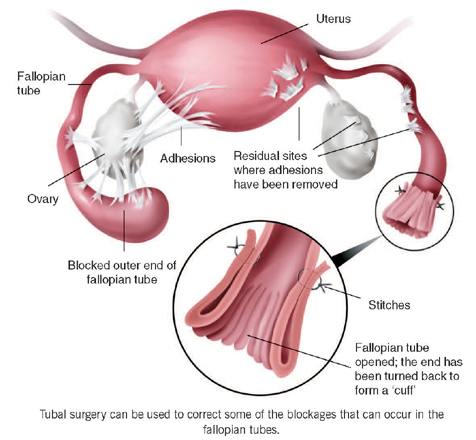
If your fallopian tubes are blocked, surgery may be necessary. Blocked fallopian tubes are often caused by an infection, usually from Chlamydia. If an infection damages the delicate lining inside the tubes, this cannot be corrected and the fallopian tubes may not be able to function normally. Sometimes, tubal surgery is indicated because of damage from endometriosis or because of scar tissue (adhesions) from previous surgery.
The tubes may be unblocked by open surgery under general anaesthesia using special microscopic techniques. Increasingly, these types of operations are being done through the laparoscope (keyhole surgery), sometimes at the time of diagnosis.
The success of surgery
The success of the surgery depends on the severity of the tubal disease. With only minor adhesions, about 50 to 60 per cent of women may conceive within 12 months. With more severe disease or tubal blockage, this may fall to only 15 to 20 per cent and, if an infection has caused the damage, the success rate may be as low as 10 per cent after 12 months.
Although surgery for more extensive tubal damage might increase a couple’s chance of success, it will usually still be unrealistically low. In this situation, IVF offers a much greater chance of pregnancy. However, if a woman’s tubes have been blocked and have swollen up with accumulated fluid secretions (a hydrosalpinx), this can reduce the chance of conception even with IVF. Surgery may then be advised to remove her fallopian tubes before any IVF treatment.
If the woman has severely damaged fallopian tubes, but the couple cannot afford IVF, she may still wish to consider surgery. Surgery may seem inappropriate because it hardly improves the chance of pregnancy. However, when there is no other way of achieving a pregnancy, even a very small chance of conception may be better than no chance.
Possible risks
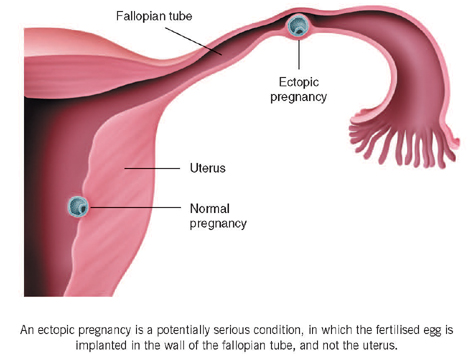
If a woman conceives after tubal surgery, there is a 10 to 15 per cent chance that the pregnancy will implant in one of her fallopian tubes (an ectopic pregnancy) rather than in the cavity of her uterus. This is a potentially serious condition that requires emergency surgery.
TREATING SPERM DISORDERS
Sperm disorders are the most common cause of subfertility. Hormone treatments and artificial insemination using the husband’s sperm (AIH) are not effective, apart from in very rare circumstances. IVF may be appropriate for treating minor disorders of sperm function, but in most cases ICSI (intracytoplasmic sperm injection) offers the best chance of pregnancy.
ICSI (intracytoplasmic sperm injection)
In most fertility clinics, the chance of pregnancy per ICSI treatment cycle varies from 12 to 30 per cent (average about 18 per cent) with live birth rates of 9 to 40 per cent (average about 25 per cent). These figures are only a few per cent lower than the results from standard IVF in couples where the man has normal sperm function.
Even for men who are not producing any sperm in their ejaculate, ICSI offers an increased chance of pregnancy if sperm can be collected surgically from the epididymes or testes. For more details about ICSI, see ‘Assisted conception’.
Sperm donation
If the man’s sperm counts are consistently low or abnormal, or he is not producing any sperm at all, the use of donor sperm may be suggested. Donor sperm may also be advised when there is a risk that a man may pass on a serious genetic disease to his children through his own sperm. Pregnancy rates are generally seven to ten per cent per cycle. The rate of conception is lower than for normal fertile couples, mainly because only freeze-stored donor sperm are used and the freezing and thawing of sperm reduces their fertilising potential.
For more on sperm donation, see ‘Egg or sperm donation’.
TREATMENT FOR ENDOMETRIOSIS
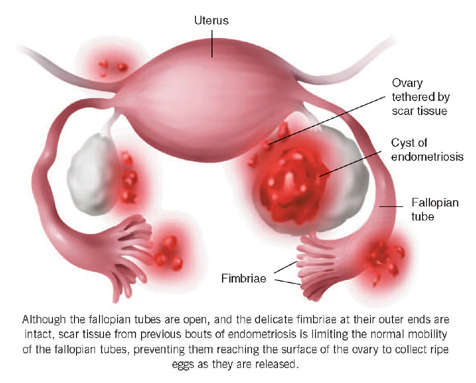
Endometriosis occurs when cells from the lining of the uterus (endometrium) are found in other places in the abdominal cavity. These cells respond to hormonal changes throughout the menstrual cycle, causing bleeding during the menstrual period. As the cells are now in an enclosed space, the blood cannot escape, as would be the case in the uterus where blood drains through the cervix. The inflammation that endometriosis causes can lead to severe abdominal pain, pelvic tenderness and painful sexual intercourse. Scarring may also occur, forming adhesions (bands of scar tissue), which can distort or block the fallopian tubes or prevent eggs passing from the ovaries to the fallopian tubes.
Treatment options
There are various drug treatments for endometriosis, usually given for several months. These may reduce endometriosis symptoms, particularly the pain. However, all the effective drug treatments have contraceptive properties while they are being taken and there is no evidence that fertility is improved after treatment.
The whole area of effective treatment for infertile women with endometriosis is a matter of some debate. Although women with endometriosis may have a reduced chance of conceiving, current evidence shows that clomifene therapy improves fertility if the couple have been trying to conceive for fewer than three years.
If minor endometriosis is diagnosed by a laparoscopy, electrical cautery or laser can be used to destroy the deposits of endometriosis. This may improve fertility in some cases. More major disease requires open surgery that is often extensive. Diathermy or laser treatment may improve pregnancy rates by 30 per cent or more after surgery. For some women with endometriosis, IVF will offer their best chance of pregnancy.